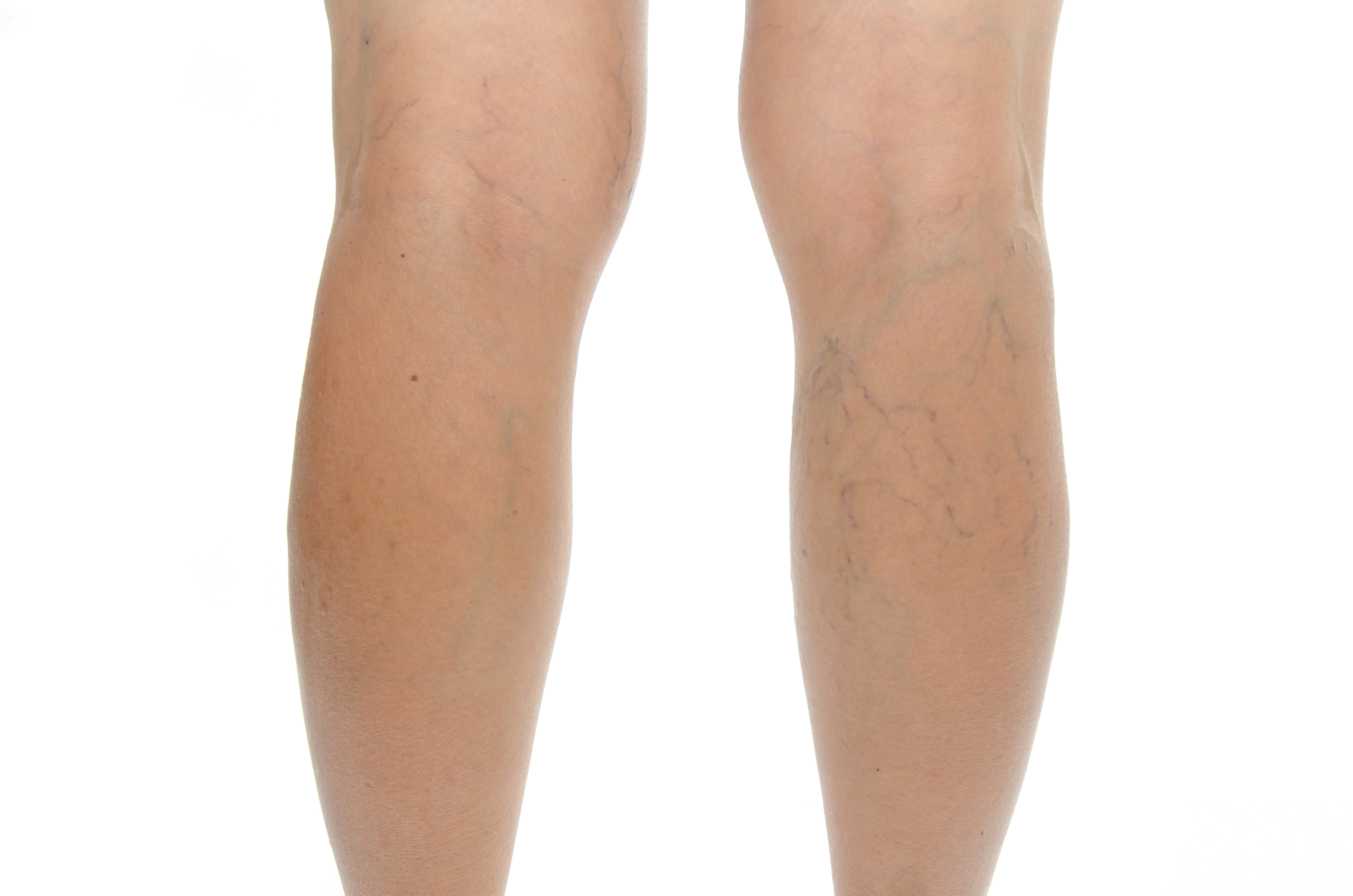
DIAGNOSIS:
The most important tools in diagnosing varicose veins are the physical examination and medical history. Varicose veins are typically diagnosed based on their appearance, and no other special tests are needed to confirm the diagnosis.
- The medical history will include questions about any vein problems, serious leg injuries, or leg ulcers you have had in the past, as well as any other risk factors you might have, including whether your family has a history of varicose veins. Talk to your doctor about any symptoms you are having (such as swelling, fatigue, or cramps in your legs) and what you have been doing to treat your symptoms, if anything.
- During the physical exam, the doctor will examine your legs and feet (or any other affected areas) for varicose veins. You will likely stand during this test. Varicose veins are usually easy to see. The doctor will also check your legs for tender areas, swelling, skin color changes, ulcers, and other signs of skin breakdown. To study the blood flow in your legs, the doctor may ask you to move your legs around in different positions.
- Ultrasound is done to see if the veins are functioning normally. This is only done when the doctor thinks this will be beneficial especially in severe varicose veins.
RECOMMENDED MEDICATIONS
Medications are not used to treat varicose veins. Thanks to less invasive procedures, varicose veins can generally be treated on an outpatient basis.
Self-care
Self-care — such as exercising, losing weight, not wearing tight clothes, elevating your legs, and avoiding long periods of standing or sitting — can ease pain and prevent varicose veins from getting worse.
Compression stockings
Wearing compression stockings is often the first approach to try before moving on to other treatments. Compression stockings are worn all day. They steadily squeeze your legs, helping veins and leg muscles move blood more efficiently. The amount of compression varies by type and brand.
Additional treatments for more-severe varicose veins
If you don’t respond to self-care, compression stockings, or if your condition is more severe, your doctor may suggest one of these varicose vein treatments:
- Sclerotherapy. In this procedure, your doctor injects small- and medium-sized varicose veins with a solution that scars and closes those veins.
- Laser surgeries. Doctors are using new technology in laser treatments to close off smaller varicose veins and spider veins.
- Catheter-assisted procedures. This procedure is usually done for larger varicose veins.
- Vein stripping. This procedure involves removing a long vein through small incisions.
- Ambulatory phlebectomy. Your doctor removes smaller varicose veins through a series of tiny skin punctures.
- Endoscopic vein surgery. You might need this operation only in an advanced case involving leg ulcers.
Varicose veins that develop during pregnancy generally improve without medical treatment within three to 12 months after delivery.